When comparing hydrocodone vs. codeine, many people aren’t sure if their pain-relieving effects will lead to addiction, especially if they’re prescribed medication for long-term chronic pain management. But not everyone who misuses their prescriptions becomes addicted, and even individuals who take their medications as prescribed can develop a tolerance.
In this article, you’ll learn if opioid pain medication like hydrocodone or codeine can lead to addiction, how to spot signs of opioid addiction, and how the DSM-5 classifies opioid use disorder.
What is Hydrocodone?
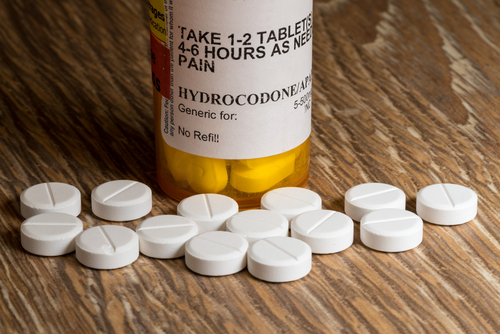
Hydrocodone belongs to a class of pharmaceuticals known as opiate analgesics, primarily prescribed for managing moderate to severe pain. The most common pain management medications with hydrocodone include Vicodin, Procet, and Maxidone.
Hydrocodone comes in a few forms including extended-release capsules and immediate-release tablets, both intended for oral consumption. The U.S. Food and Drug Administration (FDA) recently updated medical providers in 2023 to reserve hydrocodone and other opioids for severe pain that has resisted alternative treatment methods, mainly due to its abuse potential. Medical practitioners are required to meet with patients face-to-face before prescribing another batch of hydrocodone. This safeguards against any accidental misuse or overuse of this medication.
Combining hydrocodone with alcohol, other medications containing alcohol, or illicit substances can trigger grave and life-threatening side effects. However, taking more than prescribed or administering it through other means than recommended can lead to addiction and other severe side effects.
Read more: Is Oxycodone Addictive? Medication Adherence Vs. Abuse

What Is Codeine?
Codeine is another opiate analgesic and antitussive, typically prescribed to manage mild to moderate pain and cough symptoms. When codeine is used for pain relief, it changes how your brain and nervous system deal with pain. And when it’s used to calm a cough, it reduces the activity in the brain that triggers coughing.
You’ll often find codeine mixed with acetaminophen, aspirin, carisoprodol, and promethazine. It’s also used in many coughs and colds. Combination pain relief medicines with codeine include brand names such as Panadeine, Nurofen Plus, and Mersyndol, and cough relief products such as Codral and Demazin.
Many individuals who misuse codeine become used to its mild effects. They might then start misusing stronger medications to feel even stronger effects. Codeine is also abused by mixing cough syrup with soft drinks to create Lean (Purple Drank or Sizzurp).
Note: Hydrocodone and codeine are derived from the opium poppy plant, the source of heroin and fentanyl.
Are Painkillers Gateways To Addiction?
When taken as prescribed and under the direction of pain management professionals, the chances of becoming addicted to painkillers are low, but not zero. Opioids are not meant to be used for a long. For example, when an individual has surgery, they might take painkillers to manage their discomfort during the first few weeks. However, doctors don’t usually provide another prescription and recommend alternative pain management solutions, such as physical therapy or milder opioids.
When someone is taking painkillers, there’s a chance their body becomes used to the opioid’s pain-relieving effects and builds a tolerance to the prescribed dose. Once the physical need to relieve pain and the psychological need to feel better take control, an addiction develops. Some individuals can become dependent on painkillers if they have a genetic disposition or an underlying mental health disorder that relies on opioids to relieve negative emotions and feelings.
- Addiction rates for hydrocodone: Just ten years ago, 131 million Americans were prescribed hydrocodone in the form of Vicodin, often in unnecessary quantity and strength. A few years later, the FDA and DEA moved hydrocodone from a Schedule III class to Schedule II. However, there was a 7 pills-per-patient prescribing rate increase. Another report indicated that 9.3 million people were abusing and addicted to prescription opioids.
- Addiction rates for codeine: About 33 million people use Codeine every year. Unfortunately, nearly 500,000 Americans suffered fatal overdoses from powerful pain-relief medicines like Codeine between 1999 and 2019.

Taking Opioids As Prescribed
If you’re prescribed hydrocodone or codeine, here are some general rules to minimize the chance of dependence or addiction.
Taking Hydrocodone:
Individuals with pain will usually begin with a low dose of hydrocodone. If needed, your doctor may slowly raise the dose, but not more than once every 3 to 7 days. If you’re using the extended-release capsule, take it every 12 hours. For the extended-release tablet, take it once daily. Stick to a consistent time each day. Over time, your body might get used to hydrocodone. If this happens, your doctor may adjust the dose or suggest alternative pain management.
Don’t suddenly stop taking hydrocodone without consulting your doctor. Abruptly stopping might lead to withdrawal symptoms such as restlessness, irritability, anxiety, dilated pupils, watery eyes, runny nose, sleep difficulties, and more. If it’s time to reduce or stop hydrocodone, your doctor will likely decrease the dose gradually to minimize withdrawal risks.
Read more: Can You Snort Hydrocodone: The Potential Consequences
Taking Codeine:
Codeine comes in tablets, capsules, and liquid solutions. All are taken by mouth and shouldn’t be mixed with other substances. Codeine is usually taken every 4 to 6 hours for pain relief. For cough suppressant medications, follow the recommended dosage on the bottle. Read and follow the instructions on your prescription label carefully. Seek clarification from your doctor or pharmacist if any parts are unclear.
If you’ve used codeine for weeks or more, avoid stopping abruptly. Consult your doctor, who might suggest a gradual dose reduction. Suddenly discontinuing codeine could lead to withdrawal symptoms. These may include restlessness, dilated pupils, runny nose, irritability, etc.
Signs of Opioid Addiction
Individuals dealing with codeine misuse often display signs like participating in doctor shopping, drowsiness, itchy skin, fatigue, excessive sleepiness, nausea, dizziness, loss of appetite, tinted fingers, and nails, as well as constant, uncontrolled muscle twitching.
In the case of hydrocodone addiction, common symptoms encompass using street names such as “hydros,” “vics,” “vikes,” or “Vico,” engaging in doctor shopping, experiencing a slowed heart rate and breathing difficulties, feeling anxiety or depression, harboring fearfulness, undergoing sleeplessness and muscle aches during withdrawal, and even encountering seizures during an overdose.
How To Diagnose Opioid Use Disorder
According to the DSM-5, to diagnose opioid use disorder (OUD) in an individual, healthcare professionals should observe the presence of at least two of the following criteria within 12 months:
- The person often consumes opioids in larger quantities or for longer periods than initially intended.
- There is a persistent desire to cut down or control opioid use, despite unsuccessful efforts.
- A significant amount of time is dedicated to obtaining, using, or recovering from the effects of opioids.
- The individual experiences intense cravings or strong urges to use opioids.
- Opioid use results in a failure to meet important responsibilities at work, school, or home.
- Continued opioid use despite social or interpersonal problems arising from its effects.
- The person gives up or reduces participation in crucial social, occupational, or recreational activities due to opioid use.
- Opioids are used in situations that pose physical risks.
- The individual continues opioid use despite being aware of persistent physical or psychological problems caused or worsened by the substance.
- The person develops a tolerance to opioids, needing more to achieve the same effects.
- The individual experiences withdrawal symptoms when not using opioids.

Contact East Coast Recovery Center
If you or someone you know abuses hydrocodone or codeine, contact East Coast Recovery Center for opioid use disorder treatment. Even if an addiction hasn’t been going on for a long time, it’s important to catch the signs before it worsens. Our Boston, MA, treatment center has everything an individual needs to overcome opioid addiction, including individual therapy, comprehensive mental health services, provided transportation, and aftercare programs that support recovery.